
Oversleeping: How Much Rest is Too Much?
- Oversleeping is generally defined as consistently sleeping more than nine hours a night for adults, and it can be linked to various health concerns.
- Sleeping too much is associated with several health risks, including weight gain, an increased risk of heart disease, depression, cognitive impairment, and inflammation.
- Oversleeping can be a symptom of underlying medical or psychiatric conditions, such as sleep apnea, circadian rhythm disorders, or depression.
You’ve probably heard about the dangers of sleeping too little. But, did you know that it’s also possible to oversleep?
In our busy world, most public health efforts focus on the side effects of skipping slumber. As with many good things though, too much sleep poses its own health risks. It’s a complicated relationship to assess due to factors like health and aging. But, many studies find serious health implications for oversleepers.
What is Oversleeping?
First things first, let’s look at what constitutes a healthy amount of sleep.
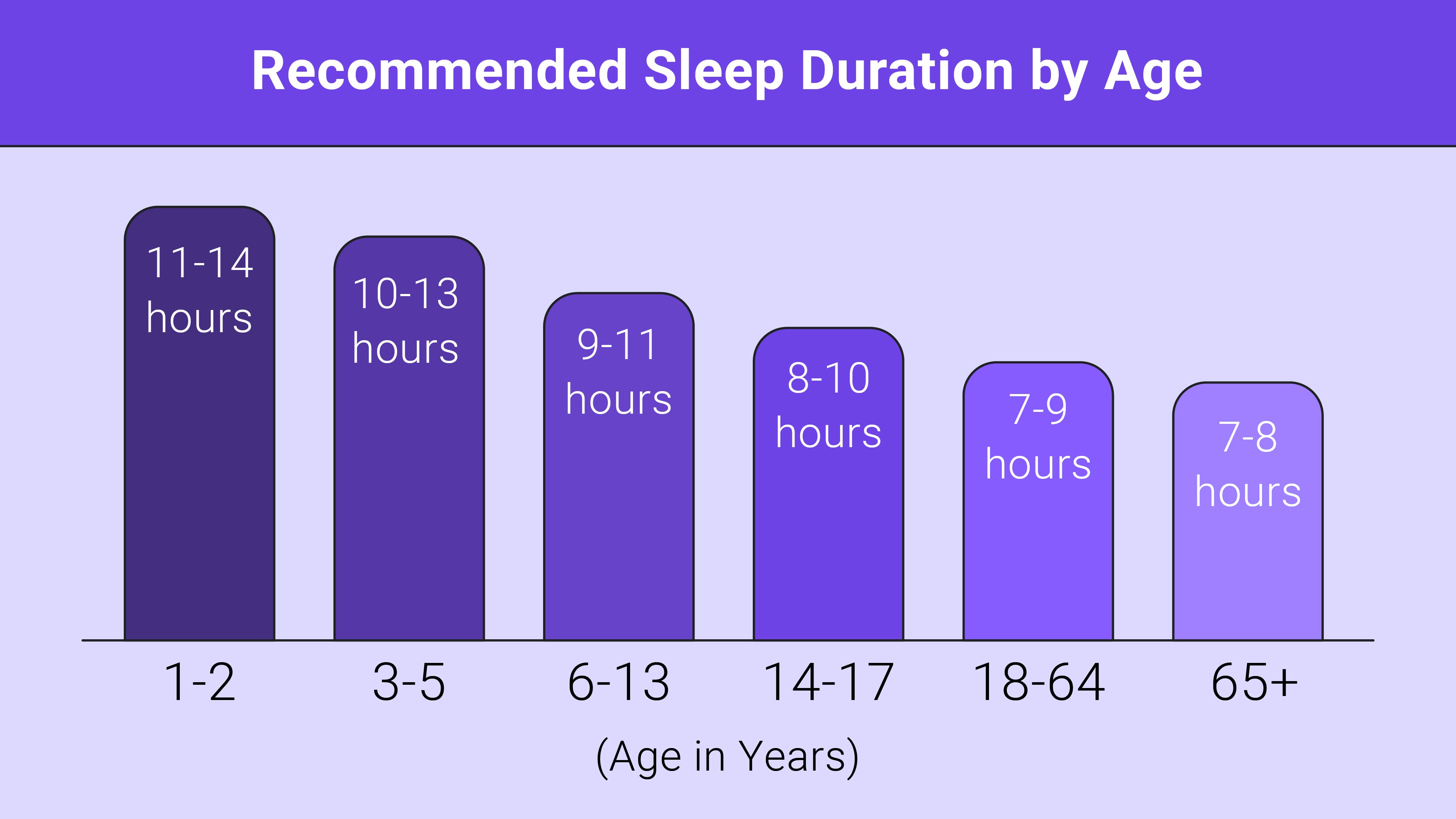
The National Sleep Foundation and most other resources define “normal” as seven to nine hours of rest per night. For adults, anything within this range is ideal. Less than seven hours risks sleep deprivation. More than nine hours is probably oversleeping.
Do you consistently clock in nine hours or more per night, most nights? If so, you might be an oversleeper.
Now this isn’t always a cause for concern. Some people’s biological clocks may predispose them to longer sleep needs. Some may have illnesses requiring more recovery time. Other people just tend to oversleep on the weekends.
Excessive Daytime Sleepiness
Also related to oversleeping is daytime drowsiness. This is feeling tired despite clocking in a healthy amount of rest. In studies, people that sleep longer than average also tend to report increased daytime sleepiness.
Daytime sleepiness can be a sign of other conditions. For example, obstructive sleep apnea can leave you drowsy during the day even if you clocked in a normal number of hours at night, and narcolepsy plunges you into sleep attacks during the day even if you got adequate sleep at night. If you sleep a normal amount of time yet still feel tired during the day, you may want to bring this up to your doctor.
The Risks of Sleeping Too Much
So, why is oversleeping a concern? Well, much like undersleeping, it turns out that it may be linked with several health concerns, according to sleep researcher Dr. Jade Wu, PhD.
“Overly long sleep is an underrated problem,” says Dr. Wu. “We all focus on sleep deprivation and getting too little sleep, but getting too much could also be a sign of a serious health problem.”
For example, physical side effects of long sleep include weight gain and the risk of heart disease. Risks of depression and neurological impairment also appear to increase with excess slumber.
Depression
The link between depression and oversleeping appears to go both ways. People with depressive symptoms are more likely to sleep longer than normal. And, people that sleep longer are more likely to experience depression.
One study of twins aimed to uncover genetic links between depression and sleep habits. Among people with normal sleep durations, they found that genes accounted for only about 27% of the variation in depressive symptoms. But, for both short and long sleeping twins (less than 7 hours or more than 9 hours), the genetic influence was much higher, at 49%. The findings suggest that oversleeping, just like undersleeping, is strongly related to depression even on a genetic level.
Impaired Cognition
Long sleep may also tie into cognitive function, particularly for adults. Among middle-age adults, one study found sleep over nine hours correlated with impaired cognition and memory. A study of Chinese people over 40 found that those who slept longest also showed the greatest cognitive impairment–people who routinely slept more than 9 hours were more than 5 times as likely to have cognitive impairment than those who usually slept 7 hours. Another found long sleepers also had greater physical impairments as well.
It may be easy to assume that age impairs the brain and triggers more sleep. One study aimed to identify influences of sleep and aging. To do so, they measured cognitive performance across a wide age span, from 15 to 89 years. Researchers found that among all ages, performance peaked at seven hours of sleep. They hypothesize that this dispels the idea that aging alone accounts for cognitive impacts of long sleep duration, and that young people’s cognition suffers from too-long sleep as well.
Researchers don’t yet know why oversleeping seems to impair cognition, or if the relationship is bi-directional. But, much like sleep deprivation, abnormal rest seems to influence the brain’s functions.
Heart Disease and Stroke
Heart disease and stroke account for one-third of deaths in the United States, according to the Centers for Disease Control and Prevention. The study of these diseases are of utmost importance to health researchers. Not only do they impact the lives of millions of people, they cost billions of dollars each year.
A study of older Chinese adults studied the effects of increases in sleep duration. They found correlations between longer sleep and increased risk of mortality. This was especially true for cardiovascular problems. A large analysis of 15 studies and habits of over 400,000 people found similar links. Both short and long sleepers had higher risk of heart disease. Another study from Japan also found increased cardiovascular mortality among elderly long sleepers.
One large review of clinical studies also found long sleepers to have the highest predictive stroke risk. Every additional hour of sleep over seven increased this risk by 13% in their findings. An American study also identified increased stroke risk for long sleepers, especially those over age 65.
Leading risk factors for these two diseases also include high blood pressure, high cholesterol, diabetes, obesity and overweight, and sedentary activity levels. Several of these factors also show links to sleep health.
Inflammation
Inflammation is a mechanism employed by the body to protect itself and heal. While useful in the short-term, chronic inflammation is associated with a range of health issues. These include higher risks of:
- Diabetes
- Cardiovascular Disease
- Arthritis
- Allergies
- Chronic Obstructive Pulmonary Disease
The chronic inflammation and the above diseases affect millions of Americans. Worldwide, chronic inflammatory diseases contribute to three in five deaths.
Studies link longer sleep, but not short sleep, with increased inflammation markers like C-reactive protein and interleukin-6.
All-Cause Mortality
All-cause mortality allows researchers to examine the overall health impact of a variable. Since sleep ties into so many systems in the body, it’s a good candidate for examination using this metric.
A study of 14,000 twins found interesting links between sleep and mortality. Both long and short durations linked with higher mortality, but in different ways. Short sleepers showed higher heritable genetic influences on mortality. However, long sleep was associated with more environmental influences on mortality.
One analysis of medical studies found that long sleep duration (but not short) was associated with a higher risk of cancer mortality as well.
Additional Risks of Long Sleep Durations

Other risks identified by research include:
- Breast Cancer: A large review of many studies that assessed sleep habits and breast cancer risk found that sleep duration over seven hours increased breast cancer risk. This was particularly true for estrogen receptor-positive breast cancer.
- Diabetes: A study of middle-age and elderly Chinese examined sleep and diabetes. They found that people sleeping more than 10 hours were 42% more likely to develop diabetes. Those sleeping over 10 hours and taking daytime naps of more than an hour were 72% more likely to develop diabetes.
- Weight Gain: One six-year study of adult sleep habits found long and short sleepers gained more weight. People sleeping more than 9 hours gained more body fat than people with 7-8 hour sleep durations.
- Kidney issues: Studies identify some links between long sleep and chronic kidney disease.
Diagnosing Oversleeping: Complex Causes
Researchers are still trying to determine if oversleeping is a cause or a symptom. But, whatever the relationship, it’s clear that abnormal sleep patterns deserve attention.
When sleeping too much begins to interfere with daily life, it’s often known clinically as “hypersomnia”. Oversleeping is also a symptom of other health conditions. These include obstructive sleep apnea (OSA) and circadian rhythm disorders.
If you feel like you’re sleeping too much or are overly tired, your doctor will seek to find out why. Usually, medical professionals will screen potential likely causes first.
This process typically involves looking at health history and lifestyle habits. Medications, diet and other factors also get addressed.
Physically, they may look for symptoms of cardiovascular or metabolic issues.
Barring physical triggers, they may screen for mental or neurological conditions. For example, excessive sleep or daytime sleepiness is often a symptom of depression.
Based on initial screening, your healthcare provider may refer you to a sleep specialist, neurologist, psychiatrist or other specialists to confirm the diagnosis.
Sleep problems are typically diagnosed using the International Classification of Sleep Disorders, Third Edition (ICSD-3). The main categories associated with the symptoms of oversleeping or excessive tiredness include:
- Central Disorders of Hypersomnolence (Hypersomnias)
- Sleep-Related Breathing Disorders (e.g. Sleep Apnea)
- Circadian Rhythm Disorders
Central Disorders of Hypersomnolence
As opposed to insomnia (which refers to having trouble falling or staying asleep), hypersomnolence is the term for longer than average need for sleep. This category comprises people that feel excessively sleepy during the day even when they’ve had enough quality sleep at night.
The central symptom of disorders in this category is excessive daytime sleepiness (EDS). EDS is characterized in the ICSD-3 as, “inability to stay awake and alert during major waking episodes of the day, resulting in periods of irrepressible need for sleep or unintended lapses into drowsiness or sleep.”
The ICSD-3 manual defines eight separate disorders in the hypersomnolence category, including primary and secondary hypersomnias.
Primary Disorders of Hypersomnolence
Excessive sleep or tiredness related to issues with the central nervous system are considered primary disorders. These include:
- Narcolepsy Type 1: Narcolepsy is characterized by an irrepressible need for sleep and daytime lapses into sleep. It is diagnosed by low levels of hypocretin in the cerebrospinal fluid and/or presence of cataplexy. Cataplexy is the sudden, brief loss of muscle control found in 70% of people with narcolepsy. Type 1 is typically treated with medications to prevent cataplexy and improve daytime alertness.
- Narcolepsy Type 2: The cause of Type 2 Narcolepsy is less understood. This category has the same sleepiness symptoms, but is characterized by the absence of cataplexy and normal hypocretin levels. It is typically treated by aiming to improve daytime alertness.
- Idiopathic Hypersomnia (IH): This condition is categorized by irrepressible daytime sleepiness as well. But, it also requires the presence of reduced REM sleep frequency, rapid sleep onset, and/or an average of 11 hours of sleep per 24 hours. Treatment typically focuses on increasing daytime alertness.
- Kleine-Levin Syndrome (KLS): Recurrent episodes of excessive sleep define KLS, as opposed to continuous symptoms. People may sleep excessively a few days to weeks at a time. KLS is also associated with abnormal, childish or disoriented behaviors. Disordered eating, hallucinations, and reduced inhibitions may also co-occur. Its cause and treatment are not well understood. Stimulants and mood stabilizers may be used to mitigate symptoms.
Secondary Disorders of Hypersomnolence
When hypersomnolence is a side effect of another cause, it is classified as a secondary condition. These include:
- Hypersomnia due to a medical condition: This category refers to daytime sleepiness related to other disorders. Examples include Parkinson’s disease, post-traumatic stress, endocrine disorders, dementia, or restless leg syndrome. It excludes OSA and circadian rhythm disorders, which are separate diagnoses.
- Hypersomnia associated with a psychiatric condition: Several mental health disorders may trigger excessive sleepiness. They can also be associated with increased time spent in bed. Depression, bipolar disorder, seasonal affective disorder, and others fall into this category.
- Hypersomnia due to a medication or substance: Certain substances affect sleep cycles. This, in turn, can make sleep feel less restorative, causing people to sleep longer.
- Insufficient sleep syndrome: This refers to tiredness caused by getting too little rest. It improves with getting an adequate amount of sleep, ruling out other diagnoses.
Sleep Apnea
Sleep apnea is characterized by repeatedly stopping and starting breathing while asleep. It can result from physical relaxation of the throat muscles, improper brain signalling, or both.
Symptoms include:
- Loud snoring
- Gasping for air
- Frequent waking or difficulty staying asleep
- Morning symptoms like dry mouth and headaches
- Excessive daytime sleepiness
- Difficulty paying attention during the day
- Irritability
Rest is constantly interrupted during the night for those with sleep apnea. This can mean that people feel tired and unrested, even though they technically spend a normal amount of time asleep.
In addition to tiredness, sleep apnea increases risks of many diseases. These include diabetes, high blood pressure, obesity and more.
Treating this condition usually reduces the symptoms associated with daytime tiredness and non-restorative sleep. Treatment typically involves both lifestyle components (like losing weight and side sleeping) and medical approaches (like using a continuous pressure breathing device or oral device).
Circadian Rhythm Disorders
The circadian rhythm or “biological clock” refers to the internal mechanisms that keep our bodies in sync with daily cycles. When functioning properly, it keeps us alert during the day and induces sleepiness at an appropriate time.
Several factors can cause circadian rhythms to get off sync, though. These include genetic predisposition, neurological conditions, lifestyle habits, jet lag, and shift work.
Circadian rhythm disorders may mean people sleep much earlier or later than usual or have irregular patterns. All of this can lead to feeling tired when you should feel alert or getting non-restorative rest.
Diagnosis typically involves examining sleep patterns and melatonin onset timing. Treatment may include improving bad sleep habits, changing sleep-wake scheduling, light therapy, or prescribed medicines.
Creating an Environment for Healthy Sleep

Numerous systems in the body impact alertness and sleep. This can make treating hyper-somnolence, oversleeping, and excessive tiredness quite complex. Although, most approaches involve improving daily habits around rest.
Maintaining healthy sleep hygiene can be helpful whether you get too little or too much sleep. Here are a few of the main things to be mindful of if you’re trying to get better quality rest.
Try to stick to a sleep schedule. Consistency with bedtime and waking times is one of the most important aspects of healthy rest.
- Identify times that you can stick to daily, including on the weekends. Variation of more than an hour can disturb circadian rhythms. And, it’s been scientifically demonstrated that trying to catch up on sleep over the weekend doesn’t entirely work.
- Allow time for enough sleep. Meaning, if you need eight hours to feel good and wake at 7 AM, try to be in bed by 10:30 PM.
Incorporate daily activity. Sedentary lifestyles correlate with many health problems, including poor sleep.
- Getting daily exercise is shown to improve overall sleep.
- Just hitting the gym once isn’t going to guarantee good sleep that night. Only regular exercise, over time, will improve sleep quality.
Be mindful of your diet. Eating a nutritious, balanced diet is associated with better rest and overall health.
- Sleep and nutrition intertwine in complex ways. One thing we do know is that more varied whole food diets tend to be ideal.
- Long sleep duration is associated with a less varied diet. In particular, long sleepers tend to consume:
- Less theobromine (found in chocolate and tea)
- Less lauric acid (found in coconut oil and coconut milk)
- Less choline (found in eggs, peanuts, beef, chicken)
- Fewer overall carbohydrates.
- Take a look at your food habits and see if there is room for improvement. Try to avoid caffeine, spicy meals and other stimulating foods late at night. Do opt for sleep-promoting foods and carbohydrate-rich snacks.
Use light and temperature to your advantage. Two stimuli your circadian clock relies on to sync itself are light and temperature.
- Get daily sunlight exposure, especially in the morning.
- Minimize exposure to blue-wave light in the evenings. This includes televisions, computers, and smartphones. See if your electronics offer nighttime settings meant to reduce blue light.
- Nighttime temperatures are best kept on the cool side of comfortable. A slightly cool room, between 65 and 72 degrees Fahrenheit is linked with the best rest.
- Rotate bedding seasonally as needed and wear lightweight, breathable pajamas.
Prioritize bedroom comfort. Feeling physically or mentally uncomfortable in a space can make falling asleep difficult. Discomfort can also lead to poor sleep that feels less restorative.
- Keep the bedroom clean and clutter-free. Keep things that trigger stress like bills, homework, or dirty laundry out of sight.
- Linens should be comfortable and washed regularly. In addition to feeling relaxing, this can also minimize allergens and bacteria.
- Sleep on the best mattress for your needs. Tossing and turning, painful pressure points, and back pain may mean your bed is past its expiration date.
Frequently Asked Questions
As we saw above, oversleeping isn’t a small issue. Oversleeping, like getting too little sleep, can cause issues and may even be a symptom of a larger issue. We hope our guide was helpful to you. Below you’ll find common questions people have asked about getting too much sleep, how much sleep is enough, and how to work towards healthier sleep.
How much sleep is too much?
Sleep isn’t just counted in hours. It’s important to get good quality sleep that follows a healthy “sleep architecture,” which includes about 15% deep sleep. A true good night’s sleep enables you to be alert the next day. It’s common to feel groggy when you wake up in the morning, but the grogginess should wear off in about 30 minutes if you’ve had quality sleep.
Each person’s sleep needs differ based on their bodies and genetics, and these needs also change throughout your life. Most adults sleep 6-8 hours a night. Some people are short sleepers who need less than 6 hours a night but still function well the next day. Yet, some people are long sleepers who need 10 hours of rest or more each night. Habits like these tend to run in families.
How many hours of sleep should you get each night?
Experts recommend an average of 7-9 hours of sleep for adults under 65, and about 7-8 hours for those over 65. At the same time, they also acknowledge sleep needs vary widely. The American Academy of Sleep Medicine (AASM) and the Sleep Research Society both recommend adults get about 7 hours of sleep. Habitually getting less than recommended hours of sleep can lead to chronic sleep deprivation.
If you need more than 8 hours of sleep each night, it’s recommended to sleep as much as you need to feel alert and awake the next day.
What causes excessive sleeping?
Excessive sleepiness can be due to an underlying medical or psychiatric issue, or a sleep-related disorder such as sleep apnea, hypersomnia, or a circadian rhythm disorder. It’s also sometimes due to irregular sleep-wake schedules and poor sleep habits.
Are there sleep disorders linked to oversleeping?
Some specific sleep disorders are linked with oversleeping, such as obstructive sleep apnea and various sleep-related movement disorders.
Obstructive Sleep Apnea is a sleep disorder in which breathing is intermittent and abnormal. Breathing stops and starts. Most people with sleep apnea snore off and on with breathing. People with sleep apnea do not get quality sleep. As a result, they may need to sleep longer or oversleep to feel refreshed.
Sleep-related movement disorders are associated with uncontrollable movements while sleeping. Leg pain and discomfort or the urge to move during rest is associated with restless legs syndrome. Other sleep-movement disorders include bruxism (teeth grinding). Sleep-related movement disorders cause oversleeping because it takes more hours to get good rest. The disorders interrupt quality sleep and leave a person feeling unrested.
How can I stop sleeping so much?
Oversleeping becomes a habit for many people. Creating a new sleep routine and sticking to it is the best way to stop sleeping too much.
First, talk to your doctor to see if you might have an underlying sleep disorder or other medical issues that could be causing excessive sleepiness. They should also review your medications to see if one may be causing you to be overly drowsy.
Do you get regular physical activity? Regular exercise can help you fall asleep faster and get better quality sleep. When you’re getting a good night’s rest, you won’t need to sleep as long.
Check your sleep hygiene. Do you have a regular sleep-and-wake schedule? Going to bed at the same time each night and waking at the same time each morning will help your body get into a better sleep schedule.
Conclusion and Next Steps
Getting into a good routine can help you avoid oversleeping. Try to aim for 7 to 9 hours of sleep a night. This is the suggested amount for alertness the next day and the best long-term health outcomes. Sticking to a sleep schedule and reducing the amount of time you sleep will help your body normalize. You’ll notice you feel more alert during the day, even if you spend less time in bed.
Don’t be afraid to reach out for help. Ask your doctor about your symptoms if you are feeling fatigued for an extended amount of time. Excessive tiredness or sleeping longer than usual can both be symptoms of serious conditions. Your doctor can help you find the ideal solution and get you back on track.


